7 expert tips to manage type 2 diabetes with diet


How food can help you manage diabetes
When you’re living with diabetes or are at risk of developing it, eating healthily is one of the best investments you can make. In fact, when you’re smart about your food choices, you may even be able to avoid developing diabetes, or at least prevent or delay the need for medication. Basically, what you need to do is follow the healthy eating advice that’s recommended for everyone, with a few additional considerations. Take control of your health with these helpful tips below:
Step 1: Eat regular meals and snacks, spread evenly over the day
This provides your body with a regular supply of energy and can help control blood glucose, or blood 'sugar' levels (BGLs). It’s also important to choose meals that are moderately sized and well balanced so that half your plate is filled with non-starchy veggies, a quarter with whole grains or starchy vegetables, and the final quarter with lean meat or an alternative source of protein, such as fish, eggs or tofu.

Step 2: Include carbohydrates with every meal
It's entirely possible to have diabetes and still eat carbs. Foods that contain carbohydrates are broken down to form glucose, which is our primary source of energy for our body and brain. For people living with diabetes, it’s vital to keep BGLs steady by choosing healthy types and amounts of carbohydrates. If you have diabetes, your healthcare professional will be able to advise a tailored approach for you. Healthy foods that contain carbohydrates include wholegrain bread, cereals, pasta and rice, starchy vegetables (potato, sweet potato and corn), fruit, legumes and some dairy products (milk and yoghurt).
Step 3: Consider the Glycaemic Index
The Glycaemic Index (GI) ranks carbohydrate-containing foods according to how they affect BGLs. Foods with a low GI raise BGLs more slowly and steadily than foods with a high GI.
Low-GI foods include heavy grain bread, rolled oats and muesli, pasta, corn, orange sweet potato, most legumes, low-fat milk and yoghurt, as well as some fruits.
Tip: You don’t need to cut out higher-GI foods completely—the trick is to combine them in a meal with low-GI options to help balance them out.
Step 4: Choose foods lower in total fat
The amount of fat you consume—saturated and trans fats in particular—can lead to weight gain, which may increase your cholesterol and BGLs.
To reduce your fat intake, try to choose reduced-fat dairy foods, lean meats, skinless chicken, margarine instead of butter, and limit consumption of fried takeaway foods, processed meats, pies, pre-packaged biscuits, cakes and other high-fat packaged foods.
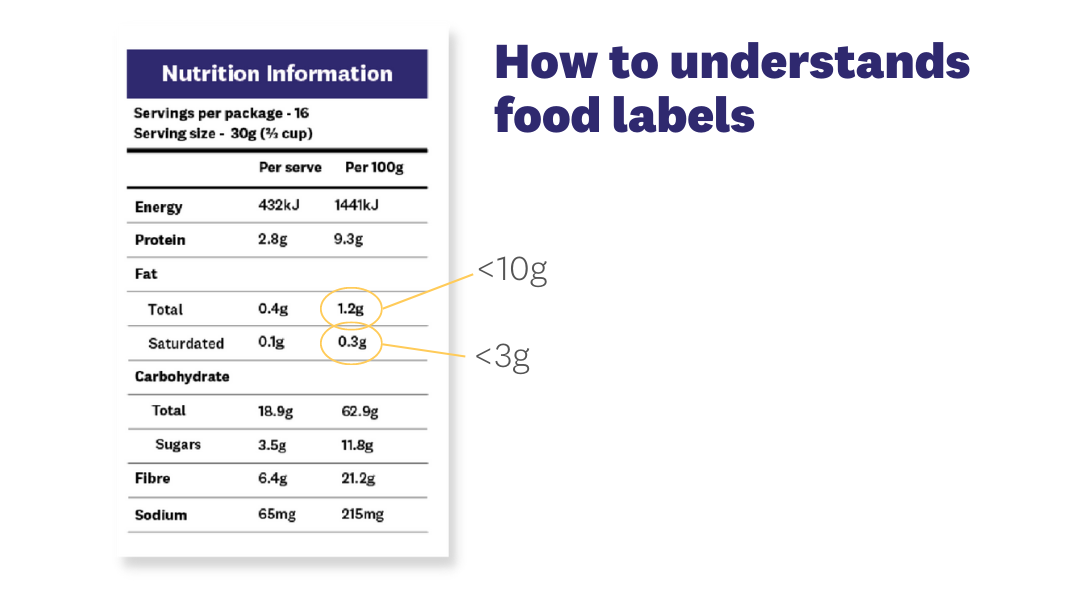
Tip: Try to check the fat content on food labels. As a general rule, try to choose foods with less than 10g of total fat per 100g, and less than 3g of saturated fat per 100g.
Step 5: Include small amounts of healthy fats
Some fat is important for good health but the key is to choose foods with healthier polyunsaturated and monounsaturated fats, such as avocado, nuts and seeds and healthy oils.
Healthy oils to include:
- Olive oil (good for pan-frying, roasting, salad dressings, marinades or drizzling over salad or pasta)
- Canola oil (good for pan-frying, stir-frying and roasting)
- Linseed/flaxseed oil (good for drizzling over soups, salads and pasta)
- Sunflower oil (good for pan-frying, stir-frying, roasting, salad dressings and marinades)

Step 6: Choose plenty of healthy high-fibre foods
Fibre has many benefits, including being important for digestive health and regular bowel movements, protecting against bowel cancer and helping to lower your BGLs and cholesterol levels.
To boost your fibre intake, choose wholegrain or high-fibre bread and cereals, and eat plenty of vegetables, legumes and fruit.
Tip: People living with diabetes should aim to eat about 25g (women) or 30g (men) of fibre per day.
Step 7: Make smarter sugar choices
Many people believe that eating too much sugar causes diabetes, but in fact, type 1 diabetes is an autoimmune condition and type 2 diabetes is caused by genetics and lifestyle, including being overweight.
However, it is important to limit foods that contain concentrated sources of sugar (such as sugar-cane products and honey) or are high in added sugar (such as soft drinks, lollies and syrups). But small amounts of sugar can be included as part of a lower-fat, low-GI, high-fibre meal for people living with diabetes. Discuss your individual approach with your healthcare professional.
