Sleep calculator: How much sleep do I need?
Your optimal amount of slumber depends on your age, lifestyle, and other factors. Here’s how to figure out your target—and finally stop tossing and turning.

Along with nutrition and physical activity, sleep is a cornerstone of good health. As researchers continue to uncover new insights about this complex biological process, it’s clear that a lot of important stuff happens when we snooze. The brain creates pathways for learning and memories, for instance, and certain tissues regenerate. By the same token, getting too little sleep is linked with a range of negative health effects. Given all that, wanting to score the best slumber possible makes sense. But how much sleep do you really need? And could a sleep calculator or high-tech gadget help you get it?
The answers depend on a range of personal factors, sleep specialists say. Here’s how to figure out the best sleep plan for you.
Recommended sleep guidelines
Let’s start with the baseline range: Most adults should aim for seven to nine hours of sleep a night to feel their best, says Douglas Kirsch, MD, FAAN, FAASM, medical director of sleep medicine at Atrium Health, a healthcare organization in Charlotte, North Carolina. Within that range, needs vary with age. The younger you are, the more ZZZs you generally need.
Sleep needs by age
You don't need a sleep calculator to get a sense of your nightly target, according to the National Sleep Foundation. Here’s a breakdown of recommended sleep durations across age brackets:
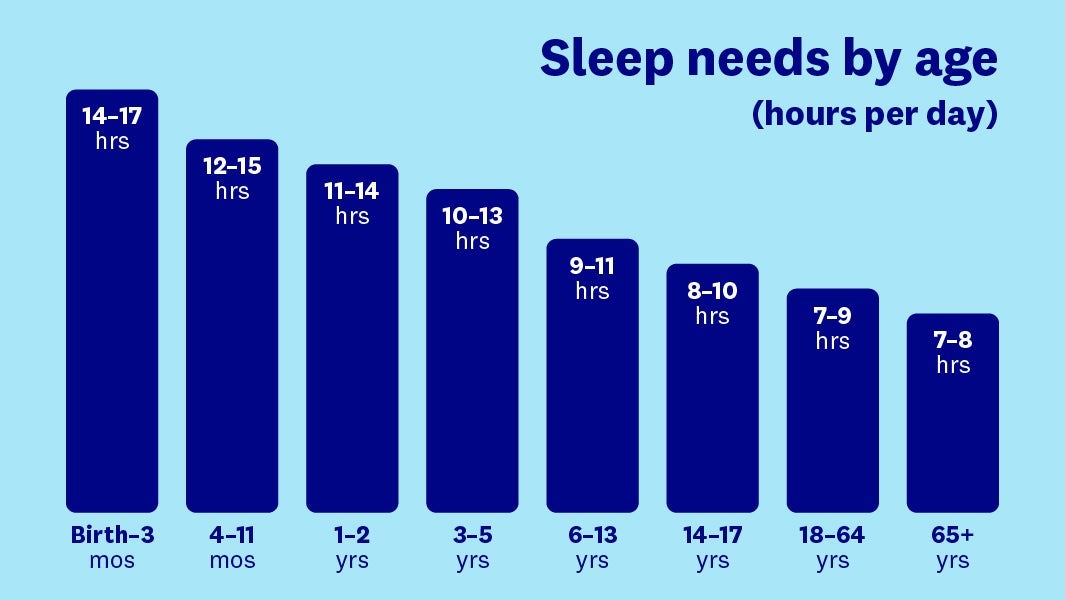
Birth to 3 months: 14–17 hours a day
4–11 months: 12–15 hours a day
1–2 years: 11–14 hours a day
3–5 years: 10–13 hours a day
6–13 years: 9–11 hours a day
14–17 years: 8–10 hours a day
18–64 years: 7–9 hours a day
65 and older: 7–8 hours a day
Common sleep challenges
More than 33% of American adults aren’t getting enough sleep, according to the Centers for Disease Control and Prevention. If you’ve ever struggled through a night (or five) of tossing and turning, you probably know that great slumber isn’t always as easy as hitting the sack and shutting off the lights. Multiple factors can interfere with sleep, from an overheated bedroom and lack of daytime physical activity to underlying issues such as sleep apnea and stress.
In broad comparisons of men and women, differences in sleep quality and quantity also crop up due to biological factors, says Mayank Shukla, MD, a sleep specialist and pulmonologist in New York City. And when sleep disruptions occur, men and women tend to respond differently. Whereas men often report physical fatigue and exhaustion after sleeping poorly, women may be more likely to report emotional effects.
Women and sleep
Hormonal activity associated with the menstrual cycle, pregnancy, and menopause can undermine sleep—for example, by causing nausea or a sensation of being overheated. Certain shifts in female hormones may also increase women’s likelihood of developing sleep disorders such as restless legs syndrome and insomnia, according to 2014 research in the Journal of Women's Health.
Nevertheless, a small 2013 study found that women tend to recover more effectively than men after a stretch of less-than-perfect shuteye—possibly due to more time spent in the deeper, restorative stages of sleep.
Men and sleep
Sleep apnea—a disorder marked by interruptions in breathing—is more common in men, possibly due to sex-based differences in fat distribution and neck circumference. Snoring also differs between sexes: An estimated 40% of men are habitual snorers, compared with just 24% of adult women, according to the American Academy of Sleep Medicine.
Men’s circadian cycles—the body’s daily rhythms of sleeping and waking—tend to run longer than women’s do, according to the National Sleep Foundation. For this reason, men may feel less tired at night.
Children and sleep
Much like adults, kids who don’t get enough sleep can have a tough time concentrating and regulating their behavior. Unlike most adults, however, children don’t always recognize when they’re exhausted, Kirsch says. In young kids, sleep trouble is often seen in bedtime resistance and middle-of-the-night waking. Adolescent sleep trouble is often seen in off-kilter circadian rhythms—think teens crashing to sleep in the wee hours and then snoozing ’til lunchtime. Overall health is another big piece of the pediatric sleep puzzle, according to a 2010 review article in the journal Psychiatry. Untreated childhood conditions including asthma, depression, and anxiety can keep kids from getting the rest they need.
Sleep calculator: What time should I go to bed and wake up?
As research on the importance of sleep continues to grow, a bevvy of apps, gadgets, and sleep calculators have hit the scene, all promising to help you achieve sweet dreams.
Many such gizmos claim to predict or sync with your sleep stages—the different phases of slumber distinguished by variables such as brain wave activity.
Other tools work more like sleep calculators. Punch in your preferred bedtime and a few other details, and an algorithm crunches the numbers to suggest an optimal time to set your alarm in the morning.
But high-tech toys and calculators might not crack the code on what you really need to feel well rested. Even among adults of the same age and sex, sleep needs vary according to environment, lifestyle, genetics, and other factors. No "perfect" number exists for any particular group of people, a 2018 review article in the journal Nature and Science of Sleep found.
So here’s what to do instead. Aim for the sleep range recommended for your age, then ask yourself some key questions: Do you wake up feeling refreshed? Are you tired throughout the day? Is tiredness keeping you from being as productive as you’d like to be? Tracking your responses against your sleep schedule may reveal useful insights particular to you.
Understanding your sleep cycle
As mentioned above, sleep isn’t a uniform state. It cycles in four distinct stages, and all are important to a truly restful experience. Sleeping with minimal interruptions supports a healthy sleep cycle.
An adult getting seven to nine hours of sleep goes through four to five sleep complete cycles per night, Kirsch says. Each lasts 90 to 120 minutes and comprises two kinds of sleep: REM (rapid eye movement) sleep, and NREM (non-rapid eye movement) sleep.
NREM sleep accounts for about 75% of all snooze time, according to the National Sleep Foundation, and happens in three stages, called N1, N2, and N3.
N1: When you’re just falling asleep or sleeping lightly.
N2: The onset of sleep. Breathing and heart rate are steady. Body temperature drops.
N3: Also known as slow-wave sleep, this stage is the most restorative, Kirsch says. Muscles relax, blood pressure drops, breathing slows, and growth and repair of tissue begins.
Next in the sleep cycle is REM sleep, which accounts for about 25% of nightly shut-eye. REM phases occur about every 90 minutes, give or take, with installments lengthening slightly as the night goes on. During REM, the body becomes relaxed and imobile, dreams occur, and as you might expect from the name of this sleep stage, eyes dart back and forth beneath the lids. The stress hormone cortisol dips. (It’ll rise again as morning approaches—a built-in alertness booster).
Why good sleep is important for health
Because adequate snooze time is important for many life processes, long-term sleep trouble may raise the risk of certain health concerns:
Weight gain: A 2017 review article in Sleep Medicine Clinics found that sleep shortfalls were linked to weight gain even when volunteers were otherwise at low risk for obesity. One possible reason may be that sleep deprivation increases appetite for high-sugar, high-fat foods, Kirsch says. While a few nights of tossing and turning are unlikely to affect weight significantly, weeks or months of poor sleep might.
Diabetes: Authors of the 2017 Sleep Medicine Clinics article note that long-term sleep loss could raise a person’s risk of developing diabetes by 33%. In addition to weight gain—a risk factor for diabetes—too little sleep may further heighten risk by setting off insulin resistance and changes to metabolic hormones.
Heart disease: Habitual sleep loss is correlated with a 20% increased likelihood of developing hypertension (a.k.a. high blood pressure), a 2013 meta-analysis in the journal Hypertension Research concluded. Losing out on sleep for a prolonged period may also increase the risk of stroke and heart attack, according to a 2010 study in the Journal of Epidemiology.
Dampened immunity: There’s growing evidence that insufficient sleep can raise the body’s susceptibility to cold viruses and interfere with the flu vaccine, Kirsch says. Inadequate sleep may influence the body’s immune response by altering production of pro-inflammatory cytokines, according to a 2017 research review in Nature and Science of Sleep.
Mental health impacts: The connection between sleep loss and mental health appears cyclical, according to the 2017 Sleep Medicine Clinics article. Some studies have determined that poor sleep can raise one’s risk of mental health concerns (such as depression); other research has found that people with mental health disorders experience sleep loss as a result of those conditions.

Best practices for a good night’s sleep
Simple adjustments to daytime habits often can make a meaningful difference in how well we sleep at night. Here are a few sleep tips to consider.
Set up a schedule. Both Kirsch and Shukla recommend going to bed and waking around the same time every day (even on weekends) to reinforce the body’s natural circadian rhythm. The more consistent you are with sleep and wake times, the more ingrained those times become in the brain—and the more likely you are to feel naturally ready for sleep when bedtime arrives.
Get your sweat on. Daily physical activity can improve sleep quality and may even be a possible remedy for insomnia, according to a 2014 research article in the American Journal of Lifestyle Medicine. Aim for about 20 minutes a day of moderate aerobic exercise—think brisk walking or a cardio class—or resistance exercises like bodyweight strength moves.
Put stress on the page. Many people’s thoughts begin racing at bedtime as they mentally review the events of the day, Kirsch says. One tip he suggests for preventing stress-induced sleep trouble: Set aside 10 minutes in the late afternoon or early evening to write down whatever’s making you feel on edge that day. Work deadlines? Family stuff? Jot it down, along with any proactive solutions you might explore. This reduces the burden on bedtime processing.
Limit coffee and alcohol at night. A couple of glasses of wine may feel relaxing in the moment; just note that consuming alcohol close to bedtime can lead to waking at odd hours of the night, Kirsch says. For this reason, he says, consider making the hours before bedtime a booze-fee zone. As for coffee, there’s probably little reason to worry about a cup or two of your favorite morning brew. Just keep the caffeine to the early parts of the day—when you normally drink it. Caffeine can interfere with sleep when consumed outside of one’s habitual zone, according to a 2018 study review published in the journal Risk Management and Healthcare Policy.
Give your smartphone a bedtime. If you’re having trouble drifting off, Instagram scrolling could be a factor. Blue light emitted by smartphones, tablets, and LCD sources can slow the body’s release of the sleep-promoting hormone melatonin. The interactive nature of social media is an added mental stimulant, Shukla adds. Set yourself for up better slumber by powering down devices 30 to 60 minutes before your bedtime.
Clear your head. Adding a few minutes of mindful breathing or meditation to your bedtime routine could help you snooze better, suggests a 2019 meta-analysis of 18 trials published in the Annals of the New York Academy of Sciences. It’s easy to do on your own—just find a quiet spot to sit, close your eyes, and focus on your breaths—or try a quick guided meditation exercise.
If you’re following good sleep practices and still aren’t feeling rested when you wake up in the mornings, speak with your doctor, who may recommend a sleep evaluation to reveal insights about your patterning, Shukla says.
Sleeping well means living well
Just as we carefully plan our days with times to eat, exercise, cook, work, and connect with others, our sleep deserves the same attention and structure, Shukla says. Simple sleep trackers can help you become attuned to your individual patterns; high-tech wearable sleep gadgets generally aren’t necessary. Simply knowing how much sleep you need and paying attention to how you feel are powerful tools for knowing whether you’re getting adequate rest. Sometimes, simple lifestyle changes are all you need to snooze better and improve your health. If you need additional sleep support, reach out to a physician or sleep specialist and get the ZZZs you deserve.
--
Jessica DiGiacinto is an associate editor at WeightWatchers®. A health and wellness writer and editor based out of New York, she’s contributed to Popsugar, Bulletproof 360, and Galvanized Media, among other media outlets.
--
This article was reviewed for accuracy in June 2021 by Stephanie L. Fitzpatrick, PhD, senior manager for multicultural programs at WW. The WW Science Team is a dedicated group of experts who ensure all our solutions are rooted in the best possible research.